Aortic valve sparing operations in aortic root aneurysms: remodeling or reimplantation?
Introduction
Over the past two decades, there has been a significant paradigm shift towards aortic valve sparing (AVS) operations over the more traditional method of prosthetic replacement for suitable aortic pathologies. Such operations, by virtue of preserving the patient’s native aortic valvular anatomy, carry numerous benefits, most notably the obviation of life-long anticoagulation medication and the reduced need for reoperation when compared to mechanical and biosynthetic valves.
Two main valve-sparing operations have dominated modern surgical practice: the David ‘reimplantation’ technique, whereby the entire aortic valve is preserved and securely sewn within a synthetic tube graft (1), and the Yacoub ‘remodeling’ technique, which replaces all three sinuses by means of a triple-tongue-shaped graft (2). Whether one technique is superior than the other has polarised the surgical community.
The present article summarises the recent evidence comparing remodelling and reimplantation techniques (3).
Search strategy
A thorough literature search was conducted using Medline and EMBASE for studies published between 1990 to December 2010 for the terms: valve-sparing.mp OR valve-preserving.mp OR valve reimplantation.mp OR valve remodeling.mp. Included studies must present selected outcomes of interest (such as aortic valve reoperation, postoperative aortic insufficiency, and/or survival) separately for each of the two techniques. Only the most complete set of outcomes was included from centres that publish duplicating results.
Results
In total, 392 papers were found using the reported search criteria. From these, 14 papers were identified to have provided the best information comparing the two valve-sparing techniques (4-17). No randomised controlled trials (RCT) or meta-analyses were found.
A total of 1,338 patients from 13 centres were included in this study. Operative technique was Yacoub for 606 patients and David for 732 patients (Table 1).
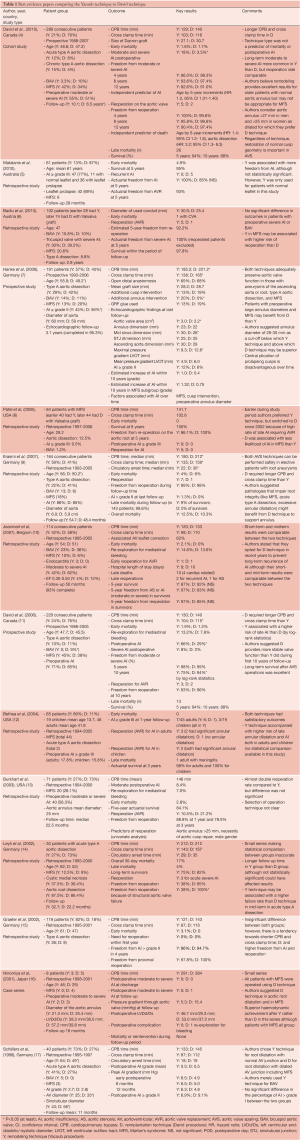
Full table
Early mortality ranged from 0-6.9% for the Yacoub technique and 0-6% for the David technique. In the largest available series of 289 patients reported by David and colleagues in 2010 (4), early mortality was 1.6% in the Yacoub cohort and 1.7% in David group. In a series of 30 patients with acute type A dissection managed with either Yacoub or David technique, the overall early mortality was 17% (14). Cardiopulmonary bypass and aortic cross clamp times were longer or equal for the David technique in all studies that reported these results (4,7,9-11,15-17).
In several series, the freedom from moderate or severe aortic insufficiency (AI) within the follow-up period was more frequent for the David technique (4,7-12,15), although it seldom reached statistical significance (4,11).
Discussion
Over the past two decades, surgical approaches to aortic root aneurysms have been repeatedly refined and improved, with progressively more complicated techniques that promised greater patient outcomes. The introduction of the composite graft procedure by Bentall in 1966 (18) has been challenged by valve-sparing techniques of David and Yacoub. These operations have surmounted the issues faced by prosthetic valves, but not without introducing limitations of their own. Such shortcomings have led to conflicting opinions regarding the suitability of these two techniques, which has yet to be thoroughly addressed.
One main issue thus far is that the selection criteria for each technique are not well established. However, based on limited evidence and personal experience, a number of surgeons have developed their own preferences over time. Some surgeons have switched from the Yacoub to the David technique (6,8) or opted for the David technique (10) over time, believing in the longer durability of this procedure. For example, Patel and associates (8) preferred the Yacoub technique for patients with the Marfan’s syndrome (MFS) up until 2002, after which they switched to the David technique due to high rate of late AI requiring reoperation. The adverse association between MFS and the remodelling method has been noted by several other authors, who suggested that using the Yacoub technique in MFS might be associated with a higher risk of reoperation for AI (4,6-9,16,17). In addition, the anatomy of the aortic valve has also impacted upon procedural choice. David et al. (4) prefers the David technique when the aortic annulus is >27 mm in men and >25 mm in women, while believing that the Yacoub technique is suitable in older patients with a normal aortic annulus. Hanke et al. (7) further suggested an annulus diameter of 28-30 mm as a dichotomous cut-off for technique selection, advocating the Yacoub technique for annuli of narrower diameters and the David technique for wider diameters.
Other factors that impact on technique selection includes acute aortic dissections, structural deficiencies, and congenital abnormalities. In a small series of 30 patients with acute type A aortic dissection managed with AVS operations, Leyh and colleagues reported a 30-day mortality rate of 17% (14). In this study, freedom from reoperation due to structural aortic valve failure was 38% in the Yacoub and 100% in the David group (P=0.04), suggesting that the Yacoub technique is associated with a higher rate of failure in mid-term acute type A dissections. Similarly, pathologies that impair root integrity (such as MFS, acute type A aortic dissection, and excessive annular dilatation) may benefit from the David rather than the Yacoub technique to support the annulus (9). Although some authors merely preferred the Yacoub technique for bicuspid aortic valve (BAV) (17), the accumulated evidence in the current study indicates comparable results for both Yacoub and David technique in BAV pathologies.
Marfan syndrome, cusp intervention, and preoperative annular diameters were also factors associated with postoperative AI in a study of 191 patients (7). In another study, an aortic annulus >25 mm, necessity of aortic cusp repair, and male gender were predictors of reoperation (13). However, David et al. (4) only identified older age as an independent predictor of postoperative AI. Taken together, this indicates that careful selection of patients for each technique and successful restoration of normal cusp geometry might omit the diameter of the aortic annulus as a predictor of postoperative AI.
The results from the present analysis demonstrate comparable outcomes for both techniques. However, there is a tendency for less freedom from significant long-term AI in the Yacoub group than the David group, which does not necessarily result in a higher reoperation rate in Yacoub group compared to the David group.
A key limitation in the present review is the difficulty in making comparisons between the two techniques. To date, no RCT has investigated the topic and there were no clear selection criteria described in most of the available reports. A concerted effort is required to more aptly compare the two techniques, so as to better improve patient selection.
In conclusion, current evidence is in favour of the David technique over the Yacoub technique in pathologies such as MFS, acute type A aortic dissection, and excessive annular dilatation, which may impair aortic root integrity. Careful selection of patients for each technique and successful restoration of normal cusp geometry are the keys to success in AVS operations.
Acknowledgements
Disclosure: The authors declare no conflict of interest.
References
- David TE, Feindel CM. An aortic valve-sparing operation for patients with aortic incompetence and aneurysm of the ascending aorta. J Thorac Cardiovasc Surg 1992;103:617-21; discussion 622.
- Sarsam MA, Yacoub M. Remodeling of the aortic valve anulus. J Thorac Cardiovasc Surg 1993;105:435-8.
- Rahnavardi M, Yan TD, Bannon PG, et al. Aortic valve-sparing operations in aortic root aneurysms: remodeling or reimplantation? Interact Cardiovasc Thorac Surg 2011;13:189-97.
- David TE, Maganti M, Armstrong S. Aortic root aneurysm: principles of repair and long-term follow-up. J Thorac Cardiovasc Surg 2010;140:S14-9; discussion S45-51.
- Matalanis G, Shi WY, Hayward PA. Correction of leaflet prolapse extends the spectrum of patients suitable for valve-sparing aortic root replacement. Eur J Cardiothorac Surg 2010;37:1311-6.
- Badiu CC, Eichinger W, Bleiziffer S, et al. Should root replacement with aortic valve-sparing be offered to patients with bicuspid valves or severe aortic regurgitation? Eur J Cardiothorac Surg 2010;38:515-22.
- Hanke T, Charitos EI, Stierle U, et al. Factors associated with the development of aortic valve regurgitation over time after two different techniques of valve-sparing aortic root surgery. J Thorac Cardiovasc Surg 2009;137:314-9.
- Patel ND, Weiss ES, Alejo DE, et al. Aortic root operations for Marfan syndrome: a comparison of the Bentall and valve-sparing procedures. Ann Thorac Surg 2008;85:2003-10; discussion 2010-1.
- Erasmi AW, Sievers HH, Bechtel JF, et al. Remodeling or reimplantation for valve-sparing aortic root surgery? Ann Thorac Surg 2007;83:S752-6; discussion S785-90.
- Jeanmart H, de Kerchove L, Glineur D, et al. Aortic valve repair: the functional approach to leaflet prolapse and valve-sparing surgery. Ann Thorac Surg 2007;83:S746-51; discussion S785-90.
- David TE, Feindel CM, Webb GD, et al. Long-term results of aortic valve-sparing operations for aortic root aneurysm. J Thorac Cardiovasc Surg 2006;132:347-54.
- Bethea BT, Fitton TP, Alejo DE, et al. Results of aortic valve-sparing operations: experience with remodeling and reimplantation procedures in 65 patients. Ann Thorac Surg 2004;78:767-72; discussion 767-72.
- Burkhart HM, Zehr KJ, Schaff HV, et al. Valve-preserving aortic root reconstruction: a comparison of techniques. J Heart Valve Dis 2003;12:62-7.
- Leyh RG, Fischer S, Kallenbach K, et al. High failure rate after valve-sparing aortic root replacement using the “remodeling technique” in acute type A aortic dissection. Circulation 2002;106 (12 Suppl 1):I229-33.
- Graeter TP, Aicher D, Langer F, et al. Mid-term results of aortic valve preservation: remodelling vs. reimplantation. Thorac Cardiovasc Surg 2002;50:21-4.
- Ninomiya M, Takamoto S, Kotsuka Y, et al. Midterm results after aortic valve-sparing operation. Jpn J Thorac Cardiovasc Surg 2001;49:706-10.
- Schäfers H, Fries R, Langer F, et al. Valve-preserving replacement of the ascending aorta: remodeling versus reimplantation. J Thorac Cardiovasc Surg 1998;116:990-6.
- Bentall H, De Bono A. A technique for complete replacement of the ascending aorta. Thorax 1968;23:338-9.





