Transcatheter aortic valve implantation in nonagenarians: selectively feasible or extravagantly futile?
Abstract
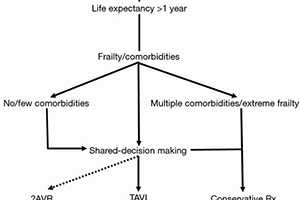
A growing number of nonagenarians is recorded as life expectancy increases. Unfortunately, this extreme-aged group is plagued by increased prevalence of aortic stenosis amidst a higher occurrence of comorbidities that pose decision dilemmas to cardiologists and cardiac surgeons when having to choose a conservative or interventional treatment modality, and a surgical or transcatheter aortic valve implantation (TAVI) approach. TAVI is an expensive procedure, which also confers a higher mortality and morbidity risk in nonagenarians, compared to younger patients. Considering the physiologic rather the chronologic age alone, and adopting a shared-decision making approach (participatory medicine), it may be more realistic to determine a patient’s candidacy for this non-surgical therapeutic modality. Thus, it practically comes down to the patient selection process by having the heart team review each nonagenarian case individually and getting the patient and the family involved, always aiming to prolong and improve patient’s quality of life (QoL), but also taking into consideration patient preferences and values, sharing and respecting goals, realistic expectations and end-of-life views and ideas. One should keep in mind that there is always the possibility that TAVI may be clinically futile for patients who have a multitude of comorbidities and extreme frailty, for whom a transition to palliative care might be prudent. Selecting nonagenarian patients with low comorbidity index and with no extreme frailty, adopting a minimalistic approach and paying attention to vascular access hemostasis may provide the elements that may lead to a successful, desirable and hopefully cost-effective outcome.
Cover