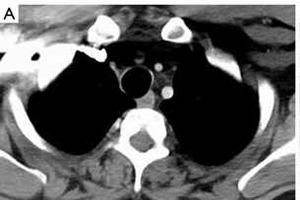
Tracheobronchoplasty for tracheomalacia
Abstract
Tracheobronchomalacia is an uncommon acquired disorder of the central airways. Common symptoms include dyspnea, constant coughing, inability to raise secretions and recurrent respiratory infections. Evaluation includes an inspiratory-expiratory chest computed tomography (dynamic CT), an awake functional bronchoscopy and pulmonary function studies. Patients with significant associated symptoms and severe collapse on CT and bronchoscopy are offered membraneous wall plication. Tracheobronchoplasty is performed through a right thoracotomy. The posterior airway is exposed after the azygous vein is ligated. The posterior wall of the trachea (and usually both main bronchi) is plicated to a sheet of thick acellular dermis (or polypropylene mesh) with a series of 4 mattress sutures of 4-0 sutures from the thoracic inlet to the bottom of the trachea to re-shape the trachea and restore the normal D shape. Patients report generally good results with improvement of their symptoms. Quality of life is usually improved while pulmonary function tests usually are not improved.
Cover