Secondary tracheal tumors: a systematic review
Abstract
Background: Secondary tracheal tumors arise from mural invasion by primary tumors in adjacent organs, metastatic lymph nodes or blood-born metastasis from distant sites. This systematic review aims to assess the presentation, management options, and clinical outcomes of these uncommon non-tracheal malignancies.
Methods: Electronic searches of the MEDLINE database were performed to identify case series and individual case reports of tracheal invasion by primary non-tracheal tumors or metastatic disease. All English-language studies with available abstracts or articles containing primary data were included.
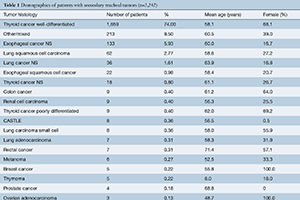
Results: From 1978 to 2017, a total of 160 case reports or case series identified 2,242 patients with invasion of the trachea by tumors of adjacent organs (n=1,853) or by metastatic lymph nodes or hematogenous spread (n=389). Common primary sites of origin were thyroid, esophagus, and lung, and the most common presentation was metachronous (range of interval: 0 to 564 months) with dyspnea, neck mass, voice change and/or hemoptysis. A majority of patients in case reports (77.9%) and case series (66.0%) underwent resection and the most common reported operation was segmental tracheal resection. Fewer patients underwent bronchoscopic intervention (21.7%) and radiation was used in 32.2% of patients. Complications after bronchoscopic treatment included bleeding, granulation tissue, and retained secretions, while anastomotic leak, unplanned tracheostomy, and new recurrent laryngeal nerve paralysis were observed after surgical resection. The rate of 30-day mortality was low (0.01–1.80%). Median survival was higher in patients with thyroid malignancy and in patients who underwent surgical management. Follow-up time ranged from 0.03 to 183 months.
Conclusions: Patients with tracheal invasion by metastatic or primary non-tracheal malignancies should be assessed for symptoms, tumor grade, tumor recurrence and concurrent metastases to decide on optimal surgical, bronchoscopic or noninterventional therapy. Clinical experience suggests that palliative endoscopic intervention for tracheal obstruction by metastasis-bearing lymph nodes is underreported.
Cover