Comparison of minimally invasive direct coronary artery bypass and drug-eluting stents for management of isolated left anterior descending artery disease: a systematic review and meta-analysis of 7,710 patients
Abstract
Background: In the contemporary era of drug-eluting stents (DES) the issue of optimal revascularization strategy for patients with isolated disease of the left anterior descending (LAD) artery has gained more significance. We aimed to evaluate the current best evidence on the subject by performing a systematic review and meta-analysis of the studies comparing minimally invasive direct coronary artery bypass (MIDCAB) grafting with DES in patients with isolated LAD disease.
Methods: A literature search was conducted from 1966 through March 2018 using MEDLINE, EMBASE, and other scientific databases to identify relevant articles. Analyzed outcomes included all-cause mortality, myocardial infarction (MI), major adverse cardiac and cerebrovascular events (MACCE) and target vessel revascularization (TVR). The random effects model was used to calculate the outcomes of both binary and continuous data to control any heterogeneity between the studies. Heterogeneity amongst the trials was determined by means of the Cochran Q value and quantified using the I2 inconsistency test. All P values were 2-sided and a 5% level was considered significant.
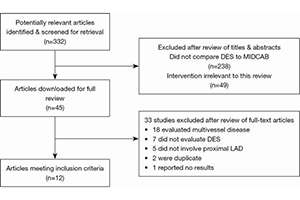
Results: A total of 7,710 patients from 12 studies were identified. There was no significant difference in mortality rate [pooled odds ratio (OR) =0.92; 95% confidence interval (CI), 0.65 to 1.32; P=0.66], MI rate (pooled OR =1.13, 95% CI, 0.62 to 2.06; P=0.69) or MACCE (pooled OR =1.31; 95% CI, 0.58 to 2.95; P=0.52). However, TVR rate was significantly more for patients having percutaneous intervention with DES (pooled OR =0.27; 95% CI, 0.16 to 0.45; P<0.0001) compared to MIDCAB.
Conclusions: MIDCAB offers superior freedom from TVR with similar mortality, MI rate, and MACCE compared to percutaneous intervention with DES for revascularization in patient with isolated proximal LAD stenosis.
Cover