Endoscopic radial artery harvesting procedure for coronary artery bypass grafting
Introduction
In patients undergoing coronary artery bypass grafting (CABG), radial arteries are the conduit graft of choice after internal thoracic arteries (1,2) because they are relatively easy to harvest and have a larger diameter than other arterial grafts. Widespread adoption of calcium channel blockers to prevent vasospasm has enhanced interest in radial arteries (3), especially in young patients in whom exclusive arterial grafting is desirable.
Complications related to conventional open radial artery harvesting are usually not negligible when they occur. The forearm is less prone to infection than the leg because of better vascular supply. Local neurological complications are infrequent and can be minimized if anatomic relations with the artery are respected and cauterization near nerves is avoided (4,5). However, harvesting usually involves an incision extending longitudinally throughout the forearm that is not cosmetically appealing.
We have recently described that endoscopic radial artery harvesting was associated with better wound appearance and less pain (6). The aim of this presentation is to describe the surgical technique of endoscopic radial artery harvesting for CABG.
Surgical techniques
General principles
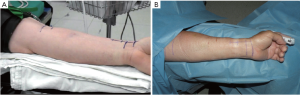
All radial arteries are harvested by specially trained physician assistants who routinely perform saphenous vein and radial artery harvesting using both open and endoscopic methods. For either operative technique, the radial artery is inspected visually before it is harvested to check for possible abnormalities that would preclude its use as a graft. The donor arm is placed on an arm board attached to the operating table, extended to approximately 80 to 90° then prepped and draped from shoulder to hand. A tourniquet is applied to the arm proximal to the elbow, then inflated only during endoscopic harvesting (7) (Figure 1A,B).
Pre-operative evaluation
When harvesting the radial artery, typically the non-dominant arm is used.
Before surgery, in order to confirm adequate collateral circulation, the pulse-assisted Allen’s test, Doppler evaluation, pulse oximetry and perfusion index, or a combination of those are performed to assess radial and ulnar arterial flow (8,9). The radial artery is not used if the Allen test is positive or the perfusion index is less than 45%. Other contraindications to radial artery harvesting include Raynaud disease, Dupuytren’s contracture, rheumatoid arthritis, scleroderma, carpal tunnel syndrome, subclavian stenosis, and renal failure requiring dialysis.
Surgical preparation
Patient positioning & preparation
Place the arm on a surgical board, positioning it at a 90° angle. For procedures using a non-sterile tourniquet, select a wide tourniquet and place the non-pressurized tourniquet high on the upper arm before prep. Shave and prep the arm, using accepted standard hospital procedure. If using a sterile tourniquet, prep and drape the arm and then place the unpressurized sterile tourniquet high on the arm.
Product assembly
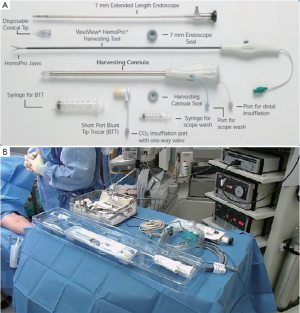
Endoscopic radial artery harvesting was introduced in our institution in 2001, but it was not until January 2002 that this technique became regularly used. It was performed using the VASOVIEW® Endoscopic Vessel Harvesting System (MAQUET Cardiovascular, Santa Clara, CA.). The 7 mm Extended Length Endoscope is attached to the camera coupler, and the light cable to the post on the endoscope. Focus the endoscope on a gauze pad and white balance the video camera, as well as ensure proper orientation of the camera head. It is important to maintain correct orientation throughout the procedure.
The conical tip is connected to the distal end of the endoscope until the proximal edge of the dissection tip lines up with the indicator etched on the endoscope shaft. The camera is focused, ensuring that the image outside the conical tip is clearly visualized. Then insert the endoscope with attached conical tip through the Blunt Tip Trocar (BTT) port. Ensure that the endoscope seal is on the BTT (Figure 2A,B).
Endoscopic technique
Incision
A 2 to 3 cm longitudinal incision is made proximal to the wrist crease over the radial artery (Figure 3). Then, using bipolar scissors or a bisector with low-energy electrocautery under direct vision, dissect locally through the lateral muscular fascia to identify the radial artery and venae comitantes which are dissected as a pedicle. The radial artery is clamped and pulse oximetry on the index finger is checked to assess radial and ulnar arterial flow. As a point of orientation, the elbow area is referred to as proximal and the wrist area is referred to as distal (Figure 4).
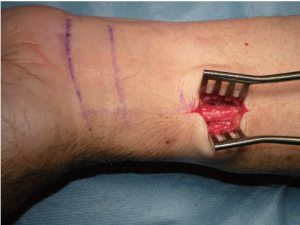
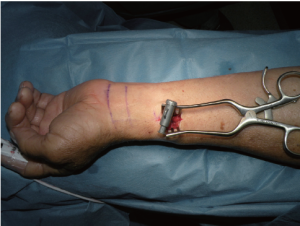
The forearm is then wrapped tightly with an Esmark bandage distal to proximal, from the fingers to the elbow in order to evacuate the blood. The tourniquet is then inflated to 75-100 mmHg over systolic blood pressure, not exceeding 250 mmHg total, and generally tourniquet time is kept under one hour. Subsequently the bandage is removed. The forearm is extended back again, and a rolled towel is placed under the wrist.
Endoscopic dissection
The radial artery is dissected as a pedicle with the accompanying venae comitantes to minimize contact with and potential spasm of the radial artery. The endoscope with the conical tip is advanced over the anterior pedicle enough to allow insertion of the BTT port. The BTT is inflated with the minimal amount of air needed to create an adequate seal. CO2 is insufflated at a pressure of 10-12 mmHg and a flow rate of 3-5 L/min to create a working tunnel (Figure 5).
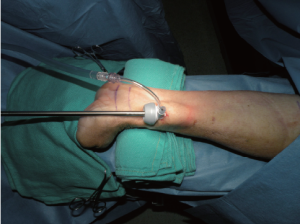
Anterior dissection
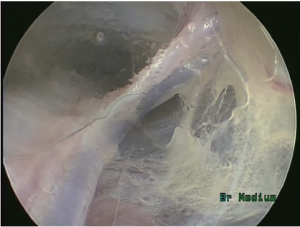
The endoscope is advanced to perform the anterior dissection along the pedicle veins on each side of the radial artery, avoiding any contact to the artery. The tissue and fascia are dissected away from the veins and radial artery, lifting the tip in an upwards direction. The lifting motion transmits shear force against the lateral muscular fascia and not the radial artery. The anterior dissection is continued to the level of the recurrent radial artery or venous plexus in the antecubital fossa (Figure 6).
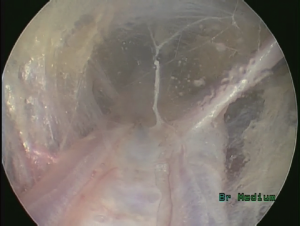
Posterior dissection
The endoscope is withdrawn to the BTT port, and is advanced posteriorly to the radial pedicle. Begin advancing the endoscope along the posterior aspect of the pedicle veins, again avoiding contact with the radial artery. The posterior branches are likely to be encountered midway up the forearm, and enough space is freed around the branch to produce minimal stress to the branch as the cannula is advanced. Continue this dissection to the level of the recurrent radial or venous plexus in the antecubital fossa (Figure 7).
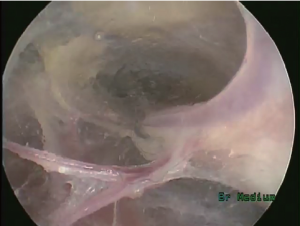
Lateral dissection
To begin the lateral dissection, the endoscope is again returned back to the BTT port. The endoscope is advanced to clear the adjoining tissue to the pedicle and to provide an adequate branch length for later sealing. Larger branches may require creating a “window” through the tissue away from the pedicle creating additional exposure for later sealing. The final goal is to obtain a pedicle-graft with both venae comitantes and the radial artery, therefore avoiding any dissection between these structures (Figure 8).
Fasciotomy
Fasciotomy of the brachioradialis muscle is performed to enhance visualization by opening up the working tunnel, and also to reduce the risk of compartment syndrome if any bleeding occurs after the endoscopic harvesting procedure. The first step is to withdraw the endoscope from the tunnel, leaving the BTT in place. The conical tip is removed from the end of the endoscope, and placed into the VasoView® HemoPro™ Endoscopic Vessel Harvesting Cannula. The VasoView® HemoPro™ Power Supply is set up between 2 to 3, and tested before use. Fasciotomy is then performed using sharp dissection, applying energy from the Power Supply to cut the tissue. Tissue dissection occurs by grasping the tissue with the jaws and then pulling and rotating the tool to apply tension while keeping view of the cut. More force can be applied when cutting fascia than when cutting vessels. The fascia should be released from the distal forearm to the mid or proximal forearm.
Branch division
Once the fasciotomy is complete, begin branch division (setting the Power Supply knob to between 2 and 3 during branch division will help the user become acclimated to the device). Capture the branches between the HemoPro Jaws by pulling the Activation Toggle into the middle position (Figure 9A). Activate the device by pulling the Activation Toggle into the proximal position, while using the C-ring to stabilize the pedicle, and monitor the pedicle during division; time of activation will depend on branch size.
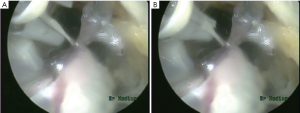
When the branch is divided, open the HemoPro™ Jaws by moving the Activation Toggle into the forward position, and retract (Figure 9B). If cutting is incomplete, reapply the jaws to the branch and repeat to the portion of the branch which is not separated.
Close the Jaws before retracting the tool into the Harvesting Cannula to avoid collision with the Cannula and Endoscope. Always inspect the site of branch division for hemostasis.
Work proximal to distal (elbow to wrist), the proximal end of the pedicle is indicated by the recurrent radial artery. Upon reaching the distal end of the pedicle, use the C-ring to run along the pedicle, ensuring that all branches have been divided and cauterized.
Division and retrieval of the radial artery
The radial artery pedicle can be divided and ligated using either the “stab and grab” technique in the antecubital fossa with an 11-blade as in the Endoscopic Vein Harvesting technique, or under endoscopic guidance using a vessel loop endoscopic technique slipknot (endoloop) of 2-0 prolene (Ethicon, Somerville, NJ). For procedures without a tourniquet, the radial pedicle should be clamped at the wrist with a soft bulldog-type clamp prior to proximal division. This is intended to keep the pedicle from back bleeding into the tunnel, but for procedures with tourniquet it is not required to clamp the radial artery.
Withdraw the pedicle in a retrograde fashion externally through the BTT port. Remove the BTT port and divide and ligate the radial artery at the wrist area using standard technique (Figure 10A,B).
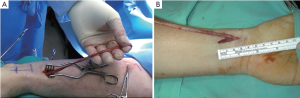
Hemostasis
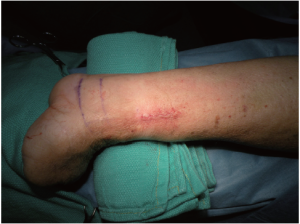
Deflate and remove the tourniquet and note the tourniquet time. Check if some spot cautery is needed to be performed for hemostasis and “milk” blood out of the tunnel. After the desired length of the artery is exposed, both ends are ligated and divided. Use a suture to close at the “stab and grab” site. The fascia and subcutaneous tissues at wrist are closed in two layers using absorbable sutures, and the skin is closed by a subcuticular method using monofilament absorbable sutures. Drains are not routinely inserted, but can be eventually placed in the subcutaneous tunnel (Figure 11).
Wrap the arm first with Kerlex and then wrap snugly with an ACE bandage. Check pulse oximetry on the thumb. Remove the ACE bandage on the first postoperative day.
Conduit preparation
The radial artery is prepared in the usual fashion and soaked and flushed with papaverine and heparinized patient blood. Clip or ligate branches as per routine surgical practice.
Comments
Endoscopic radial artery harvesting proved feasible in all patients when performed by skillful personnel. Local arm complications, such as neurological or infectious events, are infrequent and unrelated to harvesting technique. However, wound healing and pain are significantly improved after endoscopic radial artery harvesting and provides outstanding cosmetic results. This experience corroborated previous studies comparing both approaches (10,11).
Long-term patency seems to be better than for saphenous vein grafts if general principles are respected (12). Radial artery grafts are more likely to become occluded or have diffuse spasm when grafted to a coronary artery that is not severely stenotic, with a small diameter and poor distal run-off (13,14).
Careful and standardized harvesting technique plays an important role in radial artery patency (15). Other approaches aiming at enhanced flow characteristics have not gained popularity or demonstrated added benefit, such as the extrafascial technique (16) or skeletonization (17). Development and adoption of endoscopic minimally invasive saphenous vein harvesting has prompted its application to the radial artery in an effort to minimize surgical trauma.
Although the open technique is universally used in many centers, some patients are dissatisfied with the cosmetic results. More importantly, it is frequently associated with hypersensitivity of the forearm scar and hand numbness (18). Tatoulis and colleagues (19) described objective sensory loss in approximately 10% of patients, some forearm discomfort in 33%, and impaired work performance requiring rehabilitation in 8%. Those problems are usually localized to the distribution of the lateral antebrachial cutaneous nerve. Excessive traction, transection, or suturing during wound closure are the implicated mechanisms.
Although endoscopic harvesting improves patient satisfaction and acceptance (20,21), damage to the superficial radial nerve continues to be a problem for both open and endoscopic methods, producing some dorsal thenar numbness that is usually transient (20). Connolly et al. investigated neuropathy related to functional modules instead of specifying the nerve affected. Prevalence of neurologic complications was low in both groups, and no permanent deficits were detected.
Wound infection was higher than reported in other series, probably due to inclusion of superficial infections. Deeper forearm infections occurred less often with endoscopic harvesting, in accordance with other studies (22). Additionally, pain was less with endoscopic harvesting, mirroring results of previous studies on saphenous vein harvesting (23).
In addition to endoscopic harvesting taking longer than the open technique, there is also a learning curve. We, as others (24), recommend mastering saphenous vein harvesting before proceeding to the radial artery. Cost may be an issue, especially when endoscopic harvesting is performed in conjunction with saphenous vein harvesting, because the procedure requires a video tower, an ultrasonic generator, a Harmonic scalpel, and a dissector kit. However, some authors have minimized or eliminated this problem by using disposable and reusable tools (25).
There is no information on potential for mechanical or thermal injury to the conduit, particularly the endothelium. This concern is justified because of possible excessive manipulation of the conduit through a narrow tunnel. However, Shapira and colleagues have clarified this issue, proving that structural integrity and vasoreactivity of radial arteries harvested endoscopically remained intact (26).
The endoscopic radial artery harvesting technique is a safe and reproducible surgical procedure. It provides a superior cosmetic result, enhancing patient acceptability and satisfaction. Local complications are minimized, especially with regard to wound scores, pain, and infection. Neurologic complications, although reduced, could not be totally eliminated.
Acknowledgements
Disclosure: The authors declare no conflict of interest.
References
- Parolari A, Rubini P, Alamanni F, et al. The radial artery: which place in coronary operation? Ann Thorac Surg 2000;69:1288-94. [PubMed]
- Acar C, Ramsheyi A, Pagny JY, et al. The radial artery for coronary artery bypass grafting: clinical and angiographic results at five years. J Thorac Cardiovasc Surg 1998;116:981-9. [PubMed]
- Cable DG, Caccitolo JA, Pearson PJ, et al. New approaches to prevention and treatment of radial artery graft vasospasm. Circulation 1998;98:II15-21; discussion II21-2.
- Allen RH, Szabo RM, Chen JL. Outcome assessment of hand function after radial artery harvesting for coronary artery bypass. J Hand Surg Am 2004;29:628-37. [PubMed]
- Meharwal ZS, Trehan N. Functional status of the hand after radial artery harvesting: results in 3,977 cases. Ann Thorac Surg 2001;72:1557-61. [PubMed]
- Navia JL, Brozzi N, Chiu J, et al. Endoscopic versus open radial artery harvesting for coronary artery bypass grafting. J Cardiovasc Surg (Torino) 2012;53:257-63. [PubMed]
- Miles RH, Kollpainter RE, Riveron FA, et al. The pneumatic tourniquet technique for endoscopic radial artery harvest. J Card Surg 2004;19:495-8. [PubMed]
- Brodman RF, Hirsh LE, Frame R. Effect of radial artery harvest on collateral forearm blood flow and digital perfusion. J Thorac Cardiovasc Surg 2002;123:512-6. [PubMed]
- Rodriguez E, Ormont ML, Lambert EH, et al. The role of preoperative radial artery ultrasound and digital plethysmography prior to coronary artery bypass grafting. Eur J Cardiothorac Surg 2001;19:135-9. [PubMed]
- Patel AN, Henry AC, Hunnicutt C, et al. Endoscopic radial artery harvesting is better than the open technique. Ann Thorac Surg 2004;78:149-53; discussion 149-53. [PubMed]
- Kim G, Jeong Y, Cho Y, et al. Endoscopic radial artery harvesting may be the procedure of choice for coronary artery bypass grafting. Circ J 2007;71:1511-5. [PubMed]
- Desai ND, Naylor CD, Kiss A, et al. Impact of patient and target-vessel characteristics on arterial and venous bypass graft patency: insight from a randomized trial. Circulation 2007;115:684-91. [PubMed]
- Lytle BW. Prolonging patency--choosing coronary bypass grafts. N Engl J Med 2004;351:2262-4. [PubMed]
- Calafiore AM, Di Mauro M, D’Alessandro S, et al. Revascularization of the lateral wall: long-term angiographic and clinical results of radial artery versus right internal thoracic artery grafting. J Thorac Cardiovasc Surg 2002;123:225-31. [PubMed]
- Royse AG, Royse CF, Tatoulis J, et al. Postoperative radial artery angiography for coronary artery bypass surgery. Eur J Cardiothorac Surg 2000;17:294-304. [PubMed]
- Kulshrestha P, Rao L, Garb JL, et al. Use of extrafascially harvested radial artery for coronary artery revascularization: technical considerations. J Card Surg 1999;14:26-31. [PubMed]
- Amano A, Takahashi A, Hirose H. Skeletonized radial artery grafting: improved angiographic results. Ann Thorac Surg 2002;73:1880-7. [PubMed]
- Denton TA, Trento L, Cohen M, et al. Radial artery harvesting for coronary bypass operations: neurologic complications and their potential mechanisms. J Thorac Cardiovasc Surg 2001;121:951-6. [PubMed]
- Tatoulis J, Royse AG, Buxton BF, et al. The radial artery in coronary surgery: a 5-year experience--clinical and angiographic results. Ann Thorac Surg 2002;73:143-7; discussion 147-8. [PubMed]
- Connolly MW, Torrillo LD, Stauder MJ, et al. Endoscopic radial artery harvesting: results of first 300 patients. Ann Thorac Surg 2002;74:502-5; discussion 506. [PubMed]
- Casselman FP, La Meir M, Cammu G, et al. Initial experience with an endoscopic radial artery harvesting technique. J Thorac Cardiovasc Surg 2004;128:463-6. [PubMed]
- Iacò AL, Teodori G, Di Giammarco G, et al. Radial artery for myocardial revascularization: long-term clinical and angiographic results. Ann Thorac Surg 2001;72:464-8; discussion 468-9. [PubMed]
- Black EA, Campbell RK, Channon KM, et al. Minimally invasive vein harvesting significantly reduces pain and wound morbidity. Eur J Cardiothorac Surg 2002;22:381-6. [PubMed]
- Shapira OM, Eskenazi BR, Hunter CT, et al. Endoscopic versus conventional radial artery harvest--is smaller better? J Card Surg 2006;21:329-35. [PubMed]
- Newman RV, Lammle WG, Matz KJ. Cost-effective endoscopic radial artery harvesting. Ann Thorac Surg 2006;82:353-4. [PubMed]
- Shapira OM, Eskenazi BR, Anter E, et al. Endoscopic versus conventional radial artery harvest for coronary artery bypass grafting: functional and histologic assessment of the conduit. J Thorac Cardiovasc Surg 2006;131:388-94. [PubMed]