Sun’s procedure for complex aortic arch repair: total arch replacement using a tetrafurcate graft with stented elephant trunk implantation
Introduction
Patients with extensive aortic dissections or aneurysms involving the ascending aorta, aortic arch and the descending aorta remain a great challenge for many cardiovascular surgeons due to the complex surgical strategy for arch repair and the limited access to the descending aorta. A combination of surgical and endovascular techniques has enabled the development of the “stented or frozen elephant trunk” procedure (1,2), which aims to eliminate the second stage of the conventional elephant trunk or other procedures on the remaining thoracoabdominal aorta (3).
In 2002, the senior author (L.Z.S.) designed a novel stented graft (Cronus®) and proposed a modified technique of total arch replacement using a tetrafurcated graft with implantation of this new stented elephant trunk as a treatment for complex pathologies of the arch and beyond. Since its introduction in 2003, this modified technique has produced satisfactory early and long-term results (4-6). Owing to its innovative design, widespread usage and excellent outcomes, this technique was named after Dr. Sun by domestic and international colleagues in 2008 (7,8).
In this paper, we seek to demonstrate the technical essentials of the Sun’s procedure, including implantation of the stented elephant trunk, total arch replacement with a 4-branched graft, right axillary artery cannulation, selective antegrade cerebral perfusion for brain protection, moderate hypothermic circulatory arrest at 25 °C, a special sequence of arch vessel reconstruction, and early rewarming and reperfusion after distal anastomosis to minimize cerebral and cardiac ischemia (8).
Operative techniques
Exposure and cannulation
The Sun’s procedure is performed through a standard median sternotomy under cardiopulmonary bypass (CPB) and selective cerebral perfusion through the right axillary artery. General anesthesia is induced with the patient in the supine position. Blood pressure in the left radial artery and left femoral artery is monitored. We use transcranial Doppler sonography and electroencephalogram to monitor the flow velocity and electrical activity of the brain throughout the procedure. During sternotomy, great care is taken to avoid aortic rupture caused by changes in blood pressure, especially in patients with acute dissections.
The right axillary artery is our preferred inflow site for CPB. The right axillary artery is exposed through an oblique 5-8 cm incision in the right deltopectoral groove 1 cm below the clavicle, with separation of the pectoralis major muscle fibers, retraction of the pectoralis minor muscle, and careful mobilization of the adjacent vein and cords of the brachial plexus. The arterial line is bifurcated in order to perfuse the brain through the right axillary artery and the descending abdominal aorta and lower extremities through the branch of a tetrafurcate graft. In most cases, the right axillary artery can provide adequate perfusion for both brain hemispheres via the circle of Willis and extracranial collateral vessels. Other cannulae for CPB include a two-stage venous cannula placed via the right atrium and a left heart vent placed via the right superior pulmonary vein or the main pulmonary artery.
The innominate vein is mobilized and in some cases, divided for better exposure (9). The arch vessels are exposed, mobilized and surrounded. After heparinization, CPB is initiated with a flow of 2.0-2.4 L/m2/min, and systemic cooling commenced to induce hypothermia. The left phrenic and left vagus nerves are identified and protected by gentle dissection away from the anterior surface of the aorta. The distal ascending aorta is cross-clamped and cold blood cardioplegia is infused intermittently in an antegrade fashion via the coronary ostia. During the cooling phase, the ascending aorta (and the aortic root or valve in some patients) is replaced and other concomitant procedures are performed if indicated. When the nasopharyngeal temperature reaches 25 °C, the patient is put in a Trendelenburg position at a tilt of about 20 °C and circulatory arrest is instituted. After the three arch vessels are cross-clamped, antegrade cerebral perfusion through the right axillary artery is started at a flow rate of 5-10 mL/kg/min. During CPB, a mean perfusion pressure of 40-60 mmHg should be maintained. Arterial blood pH is managed with an alpha-stat strategy. A pressure of 20 mmHg or higher in the left radial artery is considered sufficient for cerebral perfusion.
Stented elephant trunk implantation
The longitudinal opening of the ascending aorta and transverse arch is extended distally to a location between the left carotid and left subclavian arteries, where the descending aorta is transected. Care should be taken to protect the vagus nerve, which lies on the surface of the distal arch. The arch vessels are transected at their origins from the aortic arch. A stented graft, Cronus® (MicroPort Medical Co. Ltd, Shanghai, China) (Figure 1), is inserted into the true lumen of the descending aorta (Figure 2) and deployed to compress the false lumen, and most importantly, to enlarge the true lumen (Figure 3). It has an extra centimeter of attached regular vascular graft on both ends, to which a conventional hand-sewn anastomosis can be performed. The delivery system consists of a grip handle, a guide wire and a pull string of 2-0 silk. During deployment, the handle is gripped in one hand, the guide wire is pulled out with the other hand, and the stent expanded automatically.
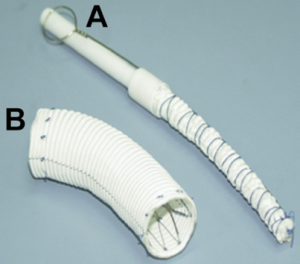
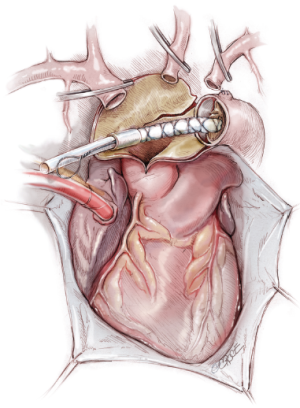
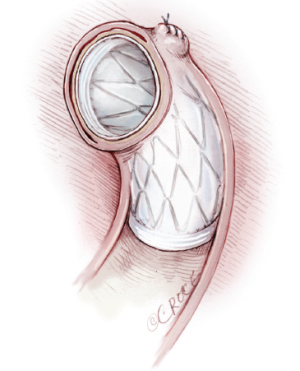
The stented graft implanted in the descending aorta is 10-15 cm in length, depending on the location of intimal tear, diameter of the aneurysmal neck, and size of the patient. In most cases, the distal end of a 10 cm stented graft will reach the level of left atrium, which can be located by preoperative computed tomography angiographic findings. For most patients with dissection, this length will suffice for closing the intimal tear located between the origin of the left subclavian artery and the descending aorta at the level of left atrium, and enlarging the true lumen of the descending aorta. In some patients with a descending aortic aneurysm, a longer 12-15 cm stented graft should be used to reach 2 cm distally beyond the aneurysmal neck.
The diameter of the stented graft should also be tailored to different aortic pathologies. In most dissection patients, we use a 24-28 mm stented graft, which is within the normal anatomic ranges of the Chinese population and can often sufficiently enlarge the true lumen, which is either severely compressed in acute settings or narrowed as a result of true lumen collapse in chronic settings. In aneurysmal patients, however, the diameter of the stented graft should be at least 15-20% greater than that of its distal neck.
The distal transverse arch is trimmed, and the stented graft is anastomosed to a 4-branched graft (Maquet Cardiovascular, Wayne, NJ) in an end-to-end fashion using continuous stitches of 3-0 or 4-0 polypropylene without pledgets. In most cases, this anastomosis is located between the left carotid and left subclavian arteries (10); this is a more superficial site than one that is distal to the left subclavian artery and allows for easier suturing and hemostasis. The suture line should include the stented graft, the native aorta and the tetrafurcate graft, so that all these structures are joined firmly together (Figure 4). When the distal anastomosis is completed, perfusion of the lower body is resumed through the perfusion limb of the tetrafurcate graft, and the CPB flow is gradually returned to 2.0-2.4 L/m2/min.
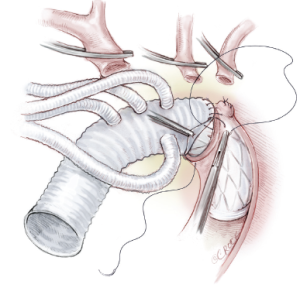
In patients with acute dissections, great care must be taken to avoid creating a new intimal tear while inserting the stent graft because the aortic wall is extremely weak and fragile. Our approach is to bend the flexible stent graft and insert it along the curvature of the arch and descending aorta so that it fits well within the true lumen, thereby reducing the risk of intimal tear. Moreover, when performing anastomoses in cases of acute dissections, we prefer using a thinner polypropylene, i.e., 4-0 for suturing the aorta, proximally and distally, and 6-0 for aortic arch branches.
Arch vessel reconstruction
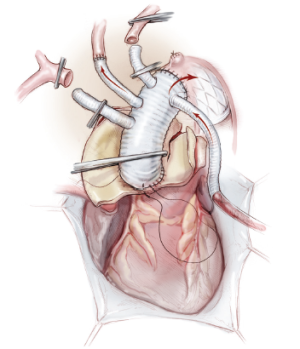
To minimize the time of cerebral and cardiac ischemia, the left common carotid artery is reconstructed first. The middle 8 mm arch branch of the tetrafurcate graft is trimmed to an appropriate length and anastomosed to the left common carotid artery end-to-end with continuous stitches of 5-0 or 6-0 polypropylene (Figure 5). Upon completion of the anastomosis, this branch of the graft is de-aired, its clamp removed and rewarming initiated, thereby enabling bilateral antegrade cerebral perfusion through both the right axillary and left common carotid arteries.

The proximal end of the tetrafurcate graft is then sutured to the ascending aortic graft in an end-to-end fashion with continuous stitches of 3-0 or 4-0 polypropylene (Figure 6). After the ascending aorta is thoroughly de-aired, the graft clamp is removed to restore coronary perfusion and cardiac activity, thus minimizing the time of myocardial ischemia. Finally, the left subclavian and innominate arteries are trimmed to an appropriate length and sutured in turn to the 8 and 10 mm branches of the 4-branched graft in an end-to-end fashion with running stitches of 5-0 or 6-0 polypropylene (Figures 7,8).
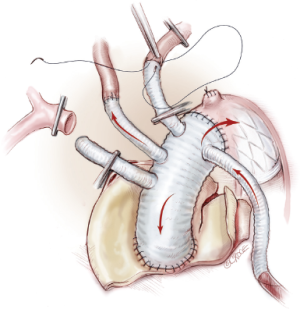
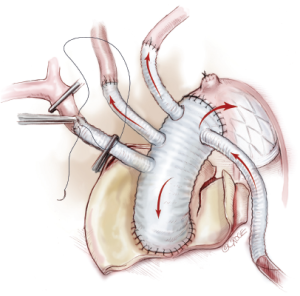
To further reduce the time of lower body ischemia, we also adopted an alternative approach for arch vessel reconstruction. Firstly, the innominate and left carotid arteries are transected at the origins from the aortic arch. Stented graft implantation, distal anastomosis, left carotid reconstruction and ascending aortic anastomosis are done in the same manner. Then, the left subclavian artery is transected 5-10 mm distal to its origin from the arch. After its proximal end is oversewn and ligated, the distal end of left subclavian artery is attached to the right 8 mm branch of the 4-branched graft end-to-end using continuous stitches of 5-0 or 6-0 polypropylene. Similarly, the innominate artery is reconstructed as previously described.
After completion of the repair and adequate rewarming, the patient is weaned from CBP, and the perfusion limb of the tetrafurcate graft is ligated and divided. For better hemostasis, we prefer approximating the residual aortic wall and in some cases, taking a pericardial patch from the patient’s native pericardium, to cover the surgical site and create a Cabrol fistula from the perigraft space to the right atrium so that any postoperative bleeding will not be problematic. Biological or chemical glue may be used to reinforce the suture lines. The remainder of the procedure, including securing hemostasis and sternal closure, is performed in a routine fashion.
Comments
The key advantage of Sun’s procedure lies in its unique stented graft, which we believe is superior to other commercially available or custom-made stented grafts, including the Chavan-Haverich (2001-2005), Jotec E-vita open and E-vita open plus (2005-2010), and the newly emerging Thoraflex Hybrid (11). The superiority of this stented graft lies in its technical simplicity, as it can be deployed very easily and quickly, often within seconds. It is highly flexible, and can tolerate the forces of bending, cross-clamping and all other surgical manipulations very well. More importantly, this special stent graft has an extra centimeter of attached regular vascular prosthesis, proximally and distally, to which a conventional hand-sewn anastomosis can be performed. This is helpful for minimizing the risk of proximal endoleak and facilitating manipulations in second-stage operations. Our results have shown that implantation of a 10-15 cm graft promotes false lumen thrombosis - which may obviate the need for surgical reintervention - and is not associated with increased incidence of paraplegia or malperfusion syndromes(4-6).
Due to the technical complexity of the frozen elephant trunk technique, some pitfalls may occur in Sun’s procedure, these include difficulties in dissecting and mobilizing the right axillary artery and arch vessels, cannulating the right axillary artery, anastomosing the left subclavian artery, and inserting the stented graft into small true lumens, as well as injury to adjacent organs and tissues (12). Specifically, extensive mobilization of a 3-5 cm segment of the left carotid artery will greatly facilitate exposure and anastomosis of the left subclavian artery. Great caution must be taken when performing the distal anastomosis between the 4-branched graft and the stented graft because bleeding at this site is very difficult to control afterwards. Each anastomosis should be inspected and selectively reinforced as needed with individual pledgetted mattress sutures to ensure hemostasis. It is important to trim and position the 4-branched graft and its arch branches appropriately so that they will not be kinked or compressed by the sternum after closure (12).
As of June 2013, we have performed Sun’s procedure in 1,092 cases, the largest series in China with an in-hospital mortality rate of 6.27% (7.98% in emergent or urgent versus 3.98% in elective cases). The incidence of second-stage operation was 4%, mostly in patients with Marfan syndrome (5). This is lower than most contemporary reports (6). At 42±18 months postoperatively, complete thrombus formation around the stented graft—extending to the diaphragmatic surface in 70% of patients—was observed in 93% of patients (5).
With increasing experience, the indications of Sun’s procedure have evolved considerably. Currently, Sun’s procedure is chiefly indicated in extensive dilating pathologies involving the ascending aorta, aortic arch, descending aorta and beyond. The most common indications include: (I) type A dissections, either with the primary entry located in the arch and descending aorta, or that involving the arch vessels, with intimal intussusception in the arch or complicated by Marfan syndrome; (II) thoracic aortic aneurysms of the ascending aorta, arch and descending aorta; (III) some type B dissections, such as those involving the aortic arch or with concomitant heart disease requiring surgical treatment and complications of endovascular repair for type B dissections, including retrograde type A dissection, endoleak, etc; (IV) congenital aortic lesions requiring repair of the arch and descending aorta (8).
At present, more than 8,000 cases of Sun’s procedure have been performed in China, and cardiac surgeons in South American countries have successfully performed this procedure in over 200 patients (8). The Sun’s procedure is now becoming increasingly applied and utilized worldwide (8), and “may become the next standard treatment in patients with type A aortic dissection involving repair of the aortic arch” (5).
Acknowledgements
Disclosure: The authors declare no conflict of interest.
References
- Kato M, Ohnishi K, Kaneko M, et al. New graft-implanting method for thoracic aortic aneurysm or dissection with a stented graft. Circulation 1996;94:II188-93. [PubMed]
- Karck M, Chavan A, Hagl C, et al. The frozen elephant trunk technique: a new treatment for thoracic aortic aneurysms. J Thorac Cardiovasc Surg 2003;125:1550-3. [PubMed]
- Borst HG, Walterbusch G, Schaps D. Extensive aortic replacement using “elephant trunk” prosthesis. Thorac Cardiovasc Surg 1983;31:37-40. [PubMed]
- Liu ZG, Sun LZ, Chang Q, et al. Should the “elephant trunk” be skeletonized? Total arch replacement combined with stented elephant trunk implantation for Stanford type A aortic dissection. J Thorac Cardiovasc Surg 2006;131:107-13. [PubMed]
- Sun L, Qi R, Zhu JM, et al. Total arch replacement combined with stented elephant trunk implantation: a new “standard” therapy for type a dissection involving repair of the aortic arch? Circulation 2011;123:971-8. [PubMed]
- Sun L, Qi R, Zhu JM, et al. Repair of acute type A dissection: our experiences and results. Ann Thorac Surg 2011;91:1147-52. [PubMed]
- Zhu XD. Preface. In: Sun LZ, Zhu JM, Liu YM, et al. eds. Surgery of the aorta (ed 1st). Beijing: People’s Medical Publishing House, 2012:5.
- Ma WG, Zheng J, Liu YM, et al. Dr. Sun’s procedure for type A aortic dissection: total arch replacement using tetrafurcate graft with stented elephant trunk implantation. Aorta 2013;1:59-64.
- Sai Sudhakar CB, Elefteriades JA. Safety of left innominate vein division during aortic arch surgery. Ann Thorac Surg 2000;70:856-8. [PubMed]
- Ziganshin B, Elefteriades JA. Does straight deep hypothermic circulatory arrest suffice for brain preservation in aortic surgery? Semin Thorac Cardiovasc Surg 2010;22:291-301. [PubMed]
- Ius F, Fleissner F, Pichlmaier M, et al. Total aortic arch replacement with the frozen elephant trunk technique: 10-year follow-up single-centre experience. Eur J Cardiothorac Surg 2013. [Epub ahead of print]. [PubMed]
- Zhu JM, Zheng J. The Sun’s procedure. In: Sun LZ, Zhu JM, Liu YM, et al. eds. Surgery of the aorta (ed 1st). Beijing: People’s Medical Publishing House, 2012:301-9.





