Hybrid arch repair in chronic B dissection
Introduction
Since its introduction in 1983 by Hans Borst, numerous variations of the classic elephant trunk technique have been introduced. Among them, the ‘frozen elephant trunk technique’ (FET) certainly represents the most innovative (1).
The FET technique, involving arch replacement and concomitant stenting of the descending thoracic aorta, has been developed as a hybrid operation to treat patients with complex pathologies of the thoracic aorta in a single stage (2).
Management of chronic type B aortic dissection is challenging. Thoracic endovascular aortic repair (TEVAR), or alternatively, open surgery through a left thoracotomy, is usually indicated in the presence of complications including dilatation or rupture (3). In addition, an uncomplicated type B dissection which dilates over time in the chronic setting can be treated during operations primarily addressing more proximal aneurysms or pathological aortic conditions.
Based on our growing experience with FET surgery, we have extended its use to selected patients with chronic type B aortic dissection. In particular, we have used this approach in patients with concomitant pathologies of the proximal aorta and when TEVAR was deemed unfeasible.
Here we show a FET procedure in a patient with a chronic type B aortic dissection and concomitant aneurysm of the aortic arch (Video 1).
The case
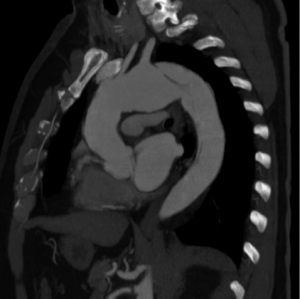
A 53-year-old man with migrating back pain was admitted to our hospital. Medical history revealed hypertension, smoking, dyslipidemia, and family history of ischemic heart disease. Computed tomography (CT) angiogram showed an acute type B aortic dissection extending to the iliac bifurcation, involving the celiac trunk and left renal artery. The entry tear was located at the proximal descending thoracic aorta, distal to the offspring of the left subclavian artery. A wide abdominal re-entry was identified at the level of the renal arteries, with the maximal diameter at the descending thoracic aorta and the aortic arch being 34 and 46 mm, respectively. Without clinical and imaging signs of impending aortic rupture, medical management was initiated and after 2 weeks, the patient was uneventfully discharged. A CT angiogram was scheduled at 4 months. This revealed a 5 mm growth of the aortic arch, a perfused false lumen without significant dimensional modifications, and obliteration of the celiac trunk (Figure 1). Coronary angiogram ruled out a significant coronary artery disease. Arch replacement with the FET technique was scheduled.
Surgical techniques
A median sternotomy was performed to approach the aorta, the arch vessels, and the heart. After systemic heparinization, a guide wire was inserted through the femoral artery in the true lumen of the descending thoracic aorta, under transesophageal echocardiographic control. The ascending aorta and the right atrium were cannulated for cardiopulmonary bypass (CPB) institution. A left ventricle drainage was inserted through the right superior pulmonary vein and cooling was initiated at nasopharyngeal temperature of 26 °C. The ascending aorta was clamped and myocardial protection achieved by means of antegrade infusion of crystalloid cardioplegia (Custodiol, Koehler Chemie, Alsbach-Haenlein, Germany). Circulatory arrest was subsequently instituted, the aortic arch was opened and antegrade selective cerebral perfusion established (10 mL/kg/min) by means of endoluminal cannulation of the arch vessels (4). The arch was completely resected and the proximal descending aorta was prepared with obliteration of the false lumen using an external Teflon felt fixed with four internal pledgetted U-stitches. The E-vita open plus delivery system was then introduced and appropriately advanced into the descending thoracic aorta over the previously positioned stiff guide-wire. The 30-mm stent graft was carefully deployed into the true lumen. The incorporated Dacron graft was pulled back and sutured to the previously prepared descending aorta using a 2/0 polypropylene running suture. After 10 minutes of lower body reperfusion, the arch vessels were re-implanted ‘en bloc’ to the E-vita open plus prosthesis. Antegrade reperfusion of the arch and thoracoabdominal aorta was then obtained by cannulating the clamped vascular graft. Rewarming was started. The proximal anastomosis to the native ascending aorta completed the aortic repair. Subsequently, CPB was easily weaned off with no need for inotropic support.
Outcome
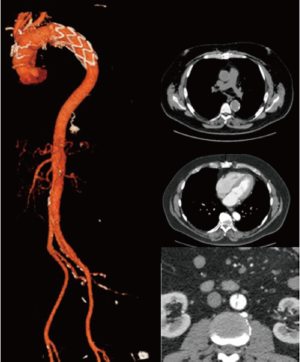
The post-operative course was uneventful. The patient was discharged on post-operative day 10 with CT angiogram showing complete thrombosis of false lumen in the descending thoracic aorta. At 4-year follow-up, CT angiogram revealed complete remodeling of the thoracic aorta; the abdominal aorta remained dissected with a patent false lumen perfused by the abdominal intimal tear (Figure 2).
Conclusions
Aortic arch replacement with the FET technique represents a valid approach in selected patients with chronic type B aortic dissection. This approach can be considered when in cases where TEVAR is unfeasible, or in patients with concomitant aortic arch (or more proximal) aneurysms.
Acknowledgements
Disclosure: The authors declare no conflict of interest.
References
- Karck M, Chavan A, Hagl C, et al. The frozen elephant trunk technique: a new treatment for thoracic aortic aneurysms. J Thorac Cardiovasc Surg 2003;125:1550-3. [PubMed]
- Di Bartolomeo R, Pacini D, Savini C, et al. Complex thoracic aortic disease: single-stage procedure with the frozen elephant trunk technique. J Thorac Cardiovasc Surg 2010;140:S81-5; discussion S86-91.
- Fattori R, Cao P, De Rango P, et al. Interdisciplinary expert consensus document on management of type B aortic dissection. J Am Coll Cardiol 2013;61:1661-78. [PubMed]
- Di Eusanio M, Schepens MA, Morshuis WJ, et al. Brain protection using antegrade selective cerebral perfusion: a multicenter study. Ann Thorac Surg 2003;76:1181-8; discussion 1188-9. [PubMed]





