Results of surgical septal myectomy for obstructive hypertrophic cardiomyopathy: the Tufts experience
Abstract
Background: For over 50 years, surgical septal myectomy has been the preferred treatment for drug-refractory heart failure symptoms in patients with obstructive hypertrophic cardiomyopathy (HCM). Over this time in the United States, the majority of myectomy operations have been performed in a small number of select referral centers.
Methods: We have taken the opportunity to report results from the relatively new Tufts HCM Center and surgical program, incorporated 13 years ago, during which 507 myectomies (52±14 years of age; 56% male) were performed by one cardiothoracic surgeon, Dr. Hassan Rastegar.
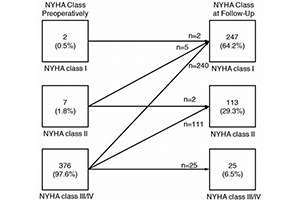
Results: Resting left ventricular (LV) outflow gradients were reduced from 56±42 mmHg preoperatively to 1.2±6.8 mmHg on most recent echocardiogram 2.0±2.5 years after surgery, and 94% of patients showed clinical improvement to NYHA functional class I or II. The first 200 myectomies were performed without mortality or major complications. Among all patients, 30-day mortality rate was 0.8%. Over follow-up of 3.2±2.8 years, 11 patients died (four due to HCM causes) with long-term survival after myectomy of 94% at 5 years (95% CI: 89–96%) and 91% at 10 years (95% CI: 84–95%), which did not differ from the age- and gender-matched general U.S. population (log-rank P=0.9).
Conclusions: This experience demonstrates that, with the appropriate support, new HCM surgical programs can provide patients successful relief of outflow obstruction, extended longevity and restored of quality of life.
Cover