Percutaneous coronary intervention versus coronary artery bypass grafting in heart transplant recipients with coronary allograft vasculopathy: a systematic review and meta-analysis of 1,520 patients
Abstract
Background: Transplant coronary artery vasculopathy (TCAV) is the major cause of late allograft failure and death in heart transplant recipients. The aim of this systematic review was to examine the outcomes of percutaneous coronary interventions (PCIs) as compared to coronary artery bypass grafting (CABG) surgery in the management of TCAV. Our secondary objective was to compare the use and outcomes of drug eluting stents (DES) as compared to bare metal stents (BMS) in this patient population.
Methods: Electronic search was performed to identify all studies in the English literature examining PCI as compared to CABG for TCAV in heart transplant recipients. All identified articles were systematically assessed for inclusion and exclusion criteria.
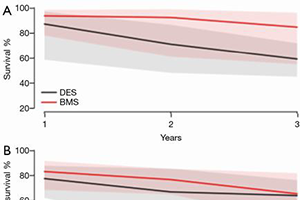
Results: Of the 4,989 studies identified, 29 studies were included. Among 1,520 patients who developed TCAV, 1,470 patients underwent PCI and 50 patients underwent CABG. There were no significant differences in baseline demographics and comorbidities among the PCI and CABG cohorts. Compared to the PCI cohort, patients who underwent CABG had a higher early mortality (CABG 36.4% vs. PCI 4.3%, P<0.001) and overall mortality (CABG 42.3% vs. PCI 21.4%, P=0.049). When comparing DES versus BMS cohorts, there were no significant differences in the rate of in-stent stenosis (DES 14.5% vs. BMS 24.4%, P=0.476), overall mortality (DES 17.4% vs. BMS 30.8%, P=0.302) or cardiac related mortality (DES 7.7% vs. BMS 21.8%, P=0.415).
Conclusions: CABG and PCI are both feasible modalities for revascularization in patients with TCAV where PCI is associated with lower mortality. There were no differences in outcomes among patients who underwent PCI with DES as compared to BMS. Potential bias may exist due to heterogeneity in available data. Further studies are needed to delineate evidence-based guidelines to tailor the appropriate therapy, CABG or PCI, to the appropriate patient.
Cover