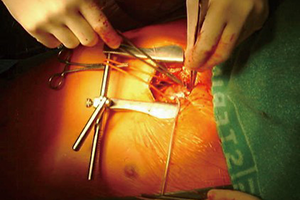
Minimally invasive primary aortic valve surgery: the OLV Aalst experience
Abstract
Background: The purpose of this study was to evaluate our in-hospital outcomes with primary J-sternotomy aortic valve surgery (JS-AVS) since the initiation of our program in 1997.
Methods: Between October 1st 1997 and August 31st 2014, 768 patients (mean age: 69.1±11.2 years, 46.6% females, 15.6% aged greater than 80 years) underwent primary JS-AVS. Additional risk factors included diabetes mellitus (n=98, 12.2%), peripheral vascular disease (n=42, 5.5%) and body mass index (BMI) greater than 30 (n=144, 18.8%). The mean logistical EuroSCORE I was 5.46%±4.5%.
Results: Aortic valve replacement and repair were performed in 758 (98.7%) and 10 (1.3%) patients respectively, for isolated valve stenosis (n=472, 61.8%), incompetence (n=56, 7.3%) and mixed valve disease (n=236, 30.9%). Valve pathology included sclerosis (n=516, 67.2%), rheumatic disease (n=110, 14.3%) and endocarditis (n=10, 1.3%). Reasons for conversion to full sternotomy (n=23, 3.0%) included porcelain ascending aorta (n=3, 0.4%), inadequate visualization (n=2, 0.3%) and intra-operative complications (n=18, 2.3%). Mean length of hospital stay was 11.0±7.4 days. Morbidity included stroke (n=15, 2.0%), revision or re-exploration (n=52, 6.8%), atrial fibrillation (AF) (n=201, 26.2%) and sternitis (n=5, 0.7%). In-hospital mortality was 1.6% (n=12). Overall survival (OS) at 30 days was 98.0%.
Conclusions: JS-AVS is safe and is our routine approach for isolated aortic valve disease (AVD). Procedure related mortality is lower than predicted, conversion rates limited and significant morbidity minimal.
Cover