Video assisted transaxillary first rib resection in treatment of thoracic outlet syndrome (TOS)
Clinical vignette
A 24-year-old woman presented with a history of swelling and heaviness in her right upper extremity following swimming or any prolonged physical activity involving overhead arm abduction. She noted occasional numbness and paresthesia. Electromyography (EMG) and nerve conduction velocity (NCV) results were normal. Venogram demonstrated high-grade narrowing of the subclavian vein at the thoracic outlet with provocative maneuvers (hyperabduction and rotation) of right upper extremity. She was referred for surgical treatment of thoracic outlet syndrome (TOS).
Surgical technique
Preparation
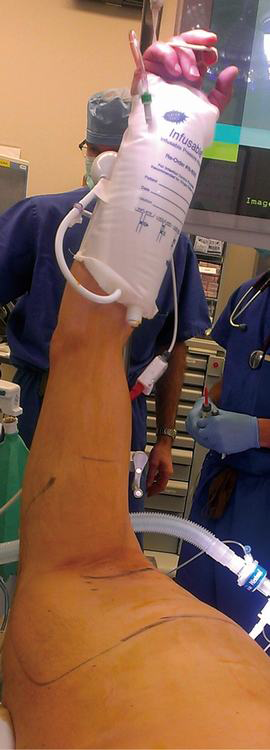
Following administration of general anesthesia, the patient was intubated with a single-lumen endotracheal tube. The patient was placed in the lateral decubitus position. A 5 pound (2.25 kg) counterweight was attached to a pulley that suspended the patient’s right arm with a padded bag. Continuous pulse oximetry monitoring of the operative side was used to assess effective circulation, as well as a surrogate for monitoring brachial plexus compression during the procedure (Figure 1). The axilla was prepped and draped.
Exposition
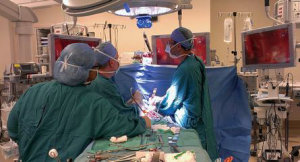
A 5-6 cm subaxillary incision was made between the latissimus dorsi and pectoralis muscles. Dissection was performed through the soft tissue to the chest wall. The surgeon stood anterior to the patient while an assistant was positioned posterior to the patient to operate the videoscope, which contained a 5 mm fiberoptic scope with a 30-degree angle of visualization (Figure 2).
Operation
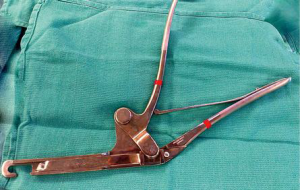
Dissection was performed on the chest wall superiorly to expose the thoracic outlet. The subclavian artery, subclavian vein and brachial plexus were identified and preserved during the procedure. Dissection was completed posteriorly to expose the posterior scalene muscles, with a portion divided for better exposure of the first rib. We avoided posterior retraction to protect the long thoracic nerve. Following division of the anterior and middle scalene muscles, the subperiosteal plane was dissected to expose the first rib. Under thoracoscopic visualization, it was divided with the first rib cutter (Figure 3), thus avoiding any injury. Resection of the remaining portions of the rib was undertaken with the rongeur both anteriorly and posteriorly (Video 1).

Completion
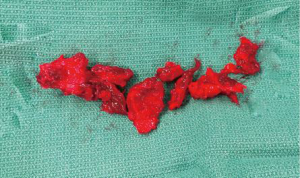
In general, we resect 90% or more of the first rib (Figure 4) to visualize the free mobilization of all thoracic outlet elements. The pleural space is not usually opened. We obtain intraoperative chest X-rays from patients prior to emergence from general anesthesia to evaluate for pneumothorax.
Comments
The subclavian artery, subclavian vein, or brachial plexus, which exit the thoracic cavity and enter the upper extremity, may be compressed and subsequently result in TOS, which has an incidence of 5-10%. Clinical manifestations of TOS may be vascular, neurologic, or both depending on the predominance of compression to the anatomic structures (1). The diagnosis of neurogenic TOS (nTOS) is confirmed by the reproduction of symptoms through provocative maneuvers. The compression mechanism is often difficult to identify; in addition to the first rib itself, the presence of a cervical rib, alterations of the costoclavicular ligament and anomalies of the scalene muscles have been identified as common factors in the etiology (1,2).
The evaluation of patients with TOS variants has been extensively reviewed in the literature (3). Initial management for most patients with nTOS is conservative, with physical therapy directed at postural correction and strengthening of the shoulder girdle. Patients with a history and examination consistent with nTOS who demonstrate improvement but not complete resolution of symptoms with physical therapy should be considered for first rib resection (2,4). While the majority of EMG and NCV tests are normal in patients with nTOS symptoms, the presence of delayed nerve conduction is another indication for surgery. For patients in whom these study results may be inconclusive or conflicting, symptomatic relief after scalene block also suggests that the patient may benefit from first rib resection. Patients with clinical and radiographically-confirmed vascular TOS should undergo first rib resection for decompression.
Sir Ashley Cooper initially described TOS in 1821 (2,5). In 1903, Bramwell recognized the first rib as the cause of TOS. In 1910, Murphy successfully resected a first rib (2,5). First rib resection via transaxillary approach is a well-established intervention with excellent exposure to the operative area. Modifications using minimally invasive surgery have been described in recent years (2,3).
We have adopted this transaxillary approach using our minimally invasive thoracic experience employing video-assisted imaging. Using the 30-degree videoscope helps to magnify and visualize all deep structures and create better exposure with a smaller incision while minimizing upper extremity traction. The resection of the first rib is performed with a first rib cutter and rongeur in a well-controlled setting.
This technique differs from previously published minimally invasive methods. We reached the first rib through the axillary incision rather than the pleural cavity (1). Our procedure prevents the need for a postoperative drain placement and may reduce the duration of hospitalization. Rather than placing a patient’s flexed elbow over their face, we prefer to stabilize the patient’s arm with the forearm extended and suspended with a padded bag and counterweight for better exposure and operative field (3). Continuous pulse oximetry of the operative side is used in addition to standard anesthesia monitoring. A diminished waveform during the operation suggests that the artery, and potentially the brachial plexus, may be compressed by instruments or stretched by retraction. When identified, this is immediately corrected in order to avoid injury. We used a 5 mm, 30-degree scope rather than a 10 mm scope (4), which occupies a smaller area. This is particularly beneficial at the time of resection, where two or more instruments (including first rib cutter or rongeur) are being used.
We believe this first rib resection technique is feasible and easy to adopt in practice. Providing a good exposure and view of deep anatomical structures allows the surgeon to plan for and perform a safer dissection, improves the performance of the assistant, and facilitates an excellent learning experience for trainees.
Acknowledgements
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
References
- Loscertales J, Congregado M, Jiménez Merchán R. First rib resection using videothorascopy for the treatment of thoracic outlet syndrome. Arch Bronconeumol 2011;47:204-7. [PubMed]
- Urschel HC Jr. The transaxillary approach for treatment of thoracic outlet syndromes. Semin Thorac Cardiovasc Surg 1996;8:214-20. [PubMed]
- Sanders RJ, Hammond SL, Rao NM. Diagnosis of thoracic outlet syndrome. J Vasc Surg 2007;46:601-4. [PubMed]
- Chan YC, Gelabert HA. High-definition video-assisted transaxillary first rib resection for thoracic outlet syndrome. J Vasc Surg 2013;57:1155-8. [PubMed]
- Barkhordarian S. First rib resection in thoracic outlet syndrome. J Hand Surg Am 2007;32:565-70. [PubMed]