Associated bare stenting of distal aorta with a Djumbodis® system versus conventional surgery in type A aortic dissection
Abstract
Background: The effectiveness of additional stenting of the distal aorta as compared to conventional surgery alone in type A aortic dissection (TAD) has yet to be proven.
Methods: We conducted this multicenter comparative study to evaluate the effects of antegrade bare stenting of the dissected aorta beyond the distal anastomosis with a Djumbodis® device system (DDS). Outcomes that were measured included early outcomes, overall mortality from aortic cause and late aortic events including re-interventions. A consecutive series of 134 patients operated on in two participating centers were distributed into study and control groups according to the treatment received: conventional surgery with DDS (DJ group, n=42) or without (control group, n=92).
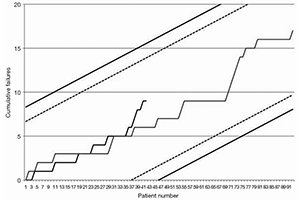
Results: Operative mortality was 21.4% and 17.6% in the DJ and control groups, respectively (P=0.9), and was within pre-specified alarm lines for both groups. In multivariate analysis, the only independent predictor of operative mortality was the presence of any complication (cardiac tamponade or malperfusion, P=0.05), which occurred more in the DJ group (OR =1.3; non-significant). Sixty patients were included into the matched survivors cohorts study (propensity scoring). The aortic event-free survival at 7 years for early survivors was 77%±10% and 48%±11% in the matched DJ group and control group, respectively (HR =0.66). Late mortality from an aortic cause was 10% and 20% in the matched DJ group and control group, respectively (RR =0.5). Actuarial freedom from aortic or vascular interventions was 71%±10% and 67%±9% in the matched DJ and control group, respectively. Operative mortality was not influenced by the use of DDS as compared to conventional surgery alone for TAD.
Conclusions: We observed a trend towards better organ perfusion in the DJ group postoperatively, and more aortic events and deaths of aortic cause in the control group during follow-up.
Cover