Parsimonious assessment for reoperative aortic valve replacement; the deterrent effect of low left ventricular ejection fraction and renal impairment
Abstract
Background: Patient comorbidities play a pivotal role in the surgical outcomes of reoperative aortic valve replacement (re-AVR). Low left ventricular ejection fraction (LVEF) and renal insufficiency (Cr >2 mg/dL) are known independent surgical risk factors. Improved preoperative risk assessment can help determine the best therapeutic approach. We hypothesize that re-AVR patients with low LVEF and concomitant renal insufficiency have a prohibitive surgical risk and may benefit from transcatheter AVR (TAVR).
Methods: From January 2002 to March 2013, we reviewed 232 patients who underwent isolated re-AVR. Patients older than 80 years were excluded to adjust for unobserved frailty. We identified 37 patients with a ≤35% LVEF (low ejection fraction group-LEF) and 195 patients with >35% LVEF (High ejection fraction group-HEF).
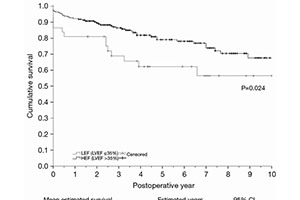
Results: The mean age was 68.4±11.5 years and there were more females (86.5% versus 64.1%, P=0.007) in the LEF group. The prevalence of renal insufficiency was higher in LEF patients (27% versus 5.6%, P=0.001). Higher operative mortality (13.5% versus 3.1%, P=0.018) was observed in the LEF group. Stroke rates were similar in both groups (8.1% versus 4.1%, P=0.39). Unadjusted cumulative survival was significantly lower in LEF patients (6.6 years, 95% CI: 5.2–8.0, versus 9.7 years, 95% CI: 8.9–10.4, P=0.024). In patients without renal insufficiency, LEF and HEF had similar survival (8.3 years, 95% CI: 7.1–9.5, versus 9.9 years, 95% CI: 9.1–10.6, P=0.90). Contrarily, in patients with renal insufficiency, LEF led to a significantly lower survival (1.1 years, 95% CI: 0.1–2.0, versus 4.8 years, 95% CI: 2.2–7.3, P=0.050). Adjusted survival analysis revealed elevations in baseline creatinine (HR =4.28, P<0.001) and LEF (HR =5.33, P=0.041) as significant predictors of long-term survival, with a significant interaction between these comorbidities (HR =7.28, P<0.001).
Conclusions: In re-AVR patients, low LVEF (≤35%) is associated with increased operative mortality. Concomitant renal insufficiency in these patients results in a prohibitively low cumulative survival. These reoperative surgical outcomes should warrant expanding the role of TAVR for reoperative patients with LEF and renal impairment.
Cover